Menstrual cramps can range from mild to quite severe. Mild menstrual cramps may be barely noticeable and of short duration sometimes felt just as a sense of light heaviness in the belly. Severe menstrual cramps can be so painful that they interfere with a woman's regular activities for several days.
How common are menstrual cramps?
Menstrual cramps of some degree affect more than an estimated 50% of women, and among these, up to 15% would describe their menstrual cramps as severe. Surveys of adolescent girls show that over 90% of girls report having menstrual cramps.
What is dysmenorrhea?
The medical term for menstrual cramps is dysmenorrhea. There are two types of dysmenorrhea, primary and secondary.
In primary dysmenorrhea, there is no underlying gynecologic problem causing the pain. This type of cramping may begin within six months to a year following menarche (the beginning of menstruation), the time when a girl starts having menstrual periods. Menstrual cramps typically do not begin until ovulatory menstrual cycles (when an egg is released from the ovaries) occur, and actual menstrual bleeding usually begins before the onset of ovulation. Therefore, an adolescent girl may not experience dysmenorrhea until months to years following the onset of menstruation.
In secondary dysmenorrhea, some underlying abnormal condition (usually involving a woman's reproductive system) contributes to the menstrual pain. Secondary dysmenorrhea may be evident at menarche but, more often, the condition develops later.
What causes menstrual cramps?
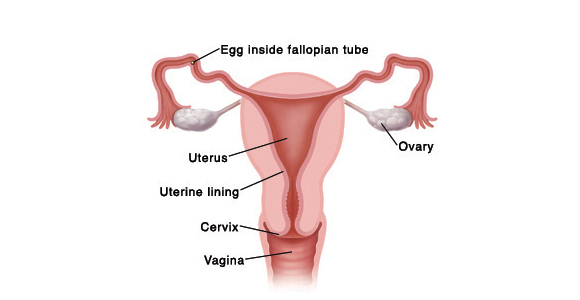
Each month, the inner lining of the uterus (the endometrium) normally builds up in preparation for a possible pregnancy. After ovulation, if the egg is not fertilized by a sperm, no pregnancy will result and the current lining of the uterus is no longer needed. The woman's estrogen and progesterone hormone levels decline, and the lining of the uterus becomes swollen and is eventually shed as the menstrual flow and is replaced by a new lining in the next monthly cycle.
When the old uterine lining begins to break down, molecular compounds called prostaglandins are released. These compounds cause the muscles of the uterus to contract. When the uterine muscles contract, they constrict the blood supply (vasoconstriction) to the endometrium. This contraction blocks the delivery of oxygen to the tissue of the endometrium which, in turn, breaks down and dies. After the death of this tissue, the uterine contractions literally squeeze the old endometrial tissue through the cervix and out of the body by way of the vagina. Other substances known as leukotrienes, which are chemicals that play a role in the inflammatory response, are also elevated at this time and may be related to the development of menstrual cramps.
Why are some cramps so painful?
Menstrual cramps are caused by the uterine contractions that occur in response to prostaglandins and other chemicals. The cramping sensation is intensified when clots or pieces of bloody tissue from the lining of the uterus pass through the cervix, especially if a woman's cervical canal is narrow.
The difference between menstrual cramps that are more painful and those that are less painful may be related to a woman's prostaglandin levels. Women with menstrual cramps have elevated levels of prostaglandins in the endometrium (uterine lining) when compared with women who do not experience cramps. Menstrual cramps are very similar to those a pregnant woman experiences when she is given prostaglandin as a medication to induce labor.
Symptoms of menstrual cramps
Menstrual cramps are pains that begin in the lower abdomen and pelvis. The discomfort can extend to the lower back or legs. The cramps can be a quite painful or simply a dull ache. They can be periodic or continual.
Menstrual cramps usually start shortly before the menstrual period, peak within 24 hours after the onset of the bleeding, and subside again after a day or two.
Menstrual cramps may be accompanied by a headache and/or nausea, which can lead, although infrequently, to the point of vomiting. Menstrual cramps can also be accompanied by either constipation or diarrhea because the prostaglandins which cause smooth muscles to contract are found in both the uterus and intestinal tract. Some women experience an urge to urinate more frequently.
Treatment for common menstrual cramps
Every woman needs to find a treatment that works for her. There are a number of possible remedies for menstrual cramps.
Current recommendations include not only adequate rest and sleep, but also regular exercise (especially walking). Some women find that abdominal massage, yoga, or orgasmic sexual activity may bring relief. A heating pad applied to the abdominal area may relieve the pain and congestion and decrease symptoms.
A number of nonprescription (over-the-counter) agents can help control the pain as well as actually prevent the menstrual cramps themselves. For mild cramps, aspirin or acetaminophen (Tylenol), or acetaminophen plus a diuretic (Diurex MPR, FEM-1, Midol, Pamprin, Premsyn, and others) may be sufficient. However, aspirin has limited effect in curbing the production of prostaglandin and is only useful for less painful cramps.
The main agents for treating moderate menstrual cramps are the nonsteroidal antiinflammatory drugs (NSAIDs), which lower the production of prostaglandin and lessen its effect. The NSAIDs that do not require a prescription are:
ibuprofen (Advil, Midol IB, Motrin, Nuprin, and others);
naproxen sodium (Aleve, Anaprox); and
ketoprofen (Actron, Orudis KT).
A woman should start taking one of these medications before her pain becomes difficult to control. This might mean starting medication 1 to 2 days before her period is due to begin and continuing taking medication 1-2 days into her period. The best results are obtained by taking one of the NSAIDs on a scheduled basis and not waiting for the pain to begin.
Prescription NSAIDs available for the treatment of menstrual cramps include mefenamic acid (Ponstel) and meclofenamate (Meclomen).
Treatment of secondary dysmenorrhea
The treatment of secondary dysmenorrhea depends on its cause. There are a number of underlying conditions which can contribute to the pain including:
endometriosis (cells from the uterine lining tare located in other areas of the body);
uterine fibroids (non-cancerous uterine growths that respond to estrogen levels);
adenomyosis (a benign condition in which the cells of the inner uterine lining invade its muscular wall, the myometrium);
pelvic inflammatory disease (PID);
Adhesions (abnormal fibrous attachments between organs); or
use of an intrauterine device (IUD) for contraception.
All of these conditions should be first diagnosed by a physician who will then recommend the optimal treatment.
If a woman begins to experience changes in her menstrual cramps, such as in their severity, timing, or location, she should consult her physician, especially if the changes are of sudden onset.